Next week we will release the latest tranche of raw data from part of our survey on coronavirus in prisons in Europe.
The project involves working with partners across a number of European countries to take stock of the current incidence and spread of coronavirus in prisons in Europe and assess the different policies and practices currently being pursued to limit the spread of coronavirus in prisons and reduce possible infections, illness and death.
The data released next week comes from the module of the survey which sought to assess the official policy responses for managing coronavirus in prisons across Europe.
The module is based on a checklist developed by the World Health Organisation (WHO) to help support policy-makers and prison administrators implement the WHO’s interim guidance on preparedness, prevention and control of COVID-19 in prisons and other places of detention.
The interim guidance contained measures recommended to prevent the virus entering prisons, to limit its spread in prisons, and to prevent transmission from within prisons to the outside community.
We launched the survey in mid-April, during the peak of the pandemic in the European epicentres. We had responses from Austria, Bulgaria, England and Wales, Hungary, Italy, Northern Ireland, Portugal, Scotland and Spain.
We originally envisaged that we would be able to easily compare the responses from each country to understand the extent to which the respective administrations had implemented the WHO checklist.
At first glance it appears as if the data shows that England and Wales and Northern Ireland have done a much better job than everyone else, and are much more transparent, with over half the recommendations fully implemented in both countries and almost no missing information.
This may well be the case, although there is more evidence in favour of that hypothesis for Northern Ireland, which scored higher for full implementation than England and Wales. Interestingly, the data for Northern Ireland suggests no transmission has occurred in prisons, whereas in England and Wales it is estimated that thousands of prisoners have been infected and 23 have died (there are of course a number of other factors which will have had an impact on this pattern, such as sizes of prison populations, proportions of older prisoners with pre-existing health conditions, different levels of testing and so on. See our COVID-19 in European prisons infographics, produced using data from the survey, for more information).
Aggregate responses to questions about how far each recommendation of the World Health Organisation's interim guidance has been implemented in different European jurisdictions.
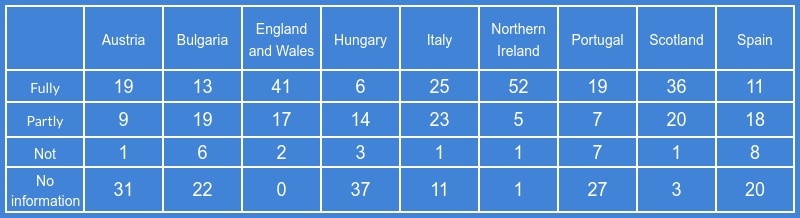
The discrepancy between the responses for these two jurisdictions and the others is in fact the result of them being collected directly from the prison administrations themselves (by CCJS, a privilege of coordinating the project) and our partners being much more restricted time-wise and so using publicly available official information, direct observation, corroborated anecdotal evidence and media reports.
Of course, all these data sources have their limitations. The variety of sources used aross jurisdictions allows us to do some quasi-triangulation to bring a critical eye to official policies and guidance, whilst retaining the benefit of releasing data much quicker than we would in a normal research project to reflect the fast pace of developments in the pandemic.
A good scour of the footnotes provided by respondents, which I have reproduced beneath the tables, reveals some useful information in this regard. For example, on the first question about whether standards of healthcare are equivalent in prisons and in the community, England and Wales and Northern Ireland are the only respondents to reply with 'fully'. The notes for Scotland and Italy indicate that this is not always the case, and give an example to explain some of the mechanics behind why it is not.
I'm obviously not trying to imply there is anything sinister going on or prison administrators are being disingenuous. On the contrary, you can see they provide many qualifications to their own responses, and they are trying very hard to keep people in prisons safe, and certainly in the case of England and Wales, in the very narrow political confines of what ministers are allowing them to do.
Instead, I think some of the responses here potentially point to the age old problem of the disconnect between policy and implementation, and in particular that the nature of prisons make it very difficult, if not impossible, to implement a comprehensively safe public health approach to a disease of this nature, especially in the context of it also being pandemic in the community.
Many jurisdictions in Europe have had the scope to embark on significant programmes of prisoner release and sentencing reform, which has certainly given them far more room to implement best practice well. Unfortunately, due to political decisions, this has not been the route taken in our own jurisdiction of England and Wales.
Here they have instead chosen to expand capacity in direct contradiction of analysis by Public Health England and HM Prison and Probation Service, who advised that the prison population should be reduced by 15,000. Apart from making future outbreaks more difficult to contain, there are all kinds of knock-on effects for prisoners and their families.
In terms of transparency, the prison administrations in England and Wales and Northern Ireland were very open to providing us with all the information we required.
It is unclear whether this is the case across the board in other European states, but given the significance of prisons as sites of transmission of COVID-19 into the community, as well as prisoners' families wanting to know they are safe from the virus, it is important that policies are publicly available and whether they adhere to the best available evidence and guidance such as that of the WHO.
Whilst the type of comparison we originally intended to carry out using this data is not feasible, as well as the conclusions I have drawn out here, it does allow us to raise some interesting questions about how specific aspects of the WHO checklist for which there was information for a given country were implemented.
These questions should form the basis for scrutiny and accountability in different European jurisdictions.
